Chapter 2: Temperature
Oral Temperature
The normal oral temperature is 35.8–37.3ºC (OER #1) or 96.4–99.1ºF. Oral temperature measurement is common and reliable because it is close to the sublingual artery. An oral thermometer is shown in Figure 2.2. The device has blue colouring, indicating that it is an oral or axillary thermometer as opposed to a rectal thermometer, which has red colouring.
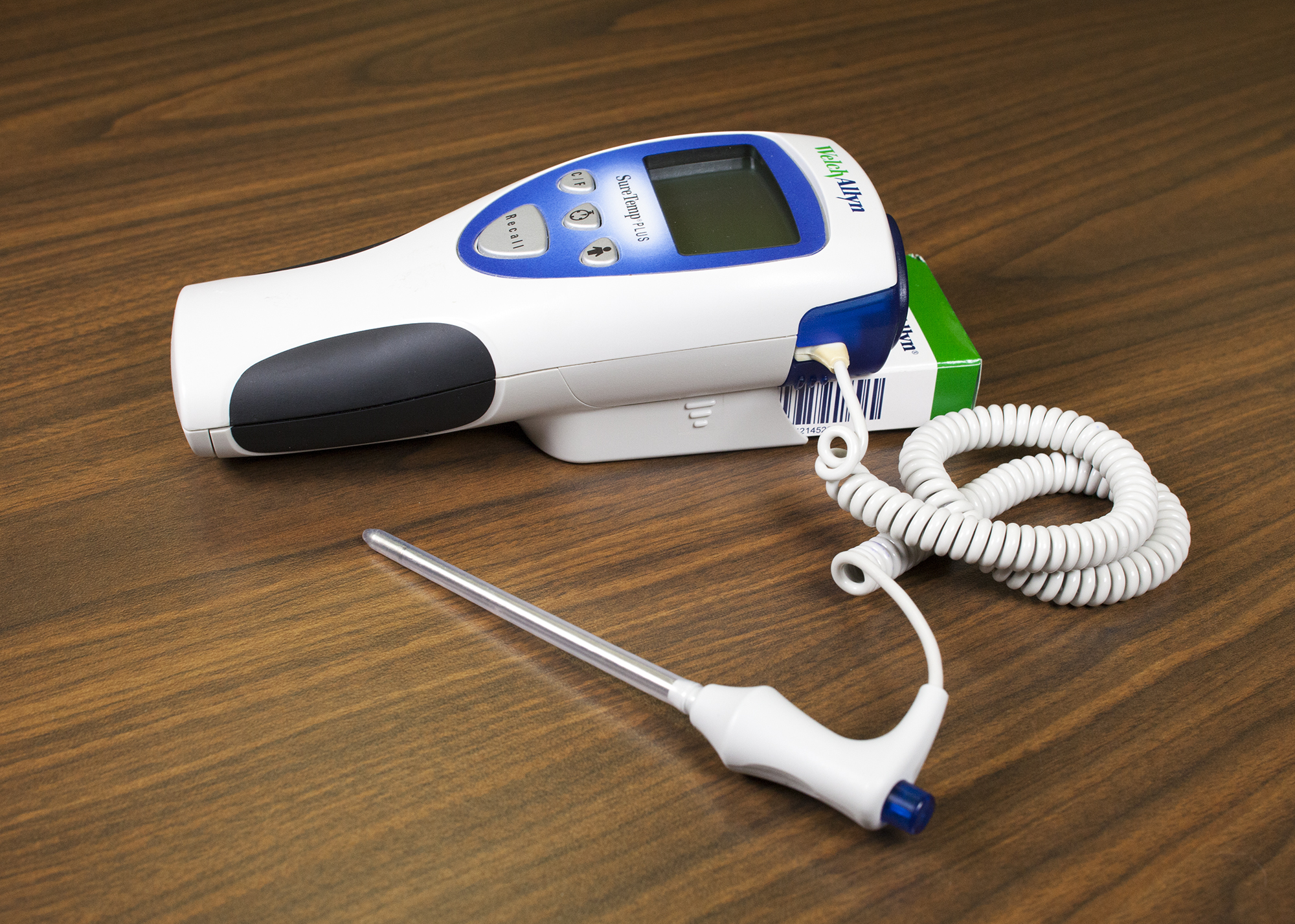
Technique
Remove the probe from the device and place a probe cover (from the box) on the oral thermometer without touching the probe cover with your hands. Place the thermometer in the client’s mouth under the tongue and instruct client to keep mouth closed and not to bite on the thermometer (OER #1). Ensure the thermometer probe is in the posterior sublingual pocket under the tongue, slightly off-centre. Leave the thermometer in place for as long as is indicated by the device manufacturer (OER #1). The thermometer will beep within a few seconds when the temperature has been taken: most oral thermometers are electronic and provide a digital display of the reading. Discard the probe cover in the garbage (without touching the cover) and place the probe back into the device. See Figure 2.3 of an oral temperature being taken.
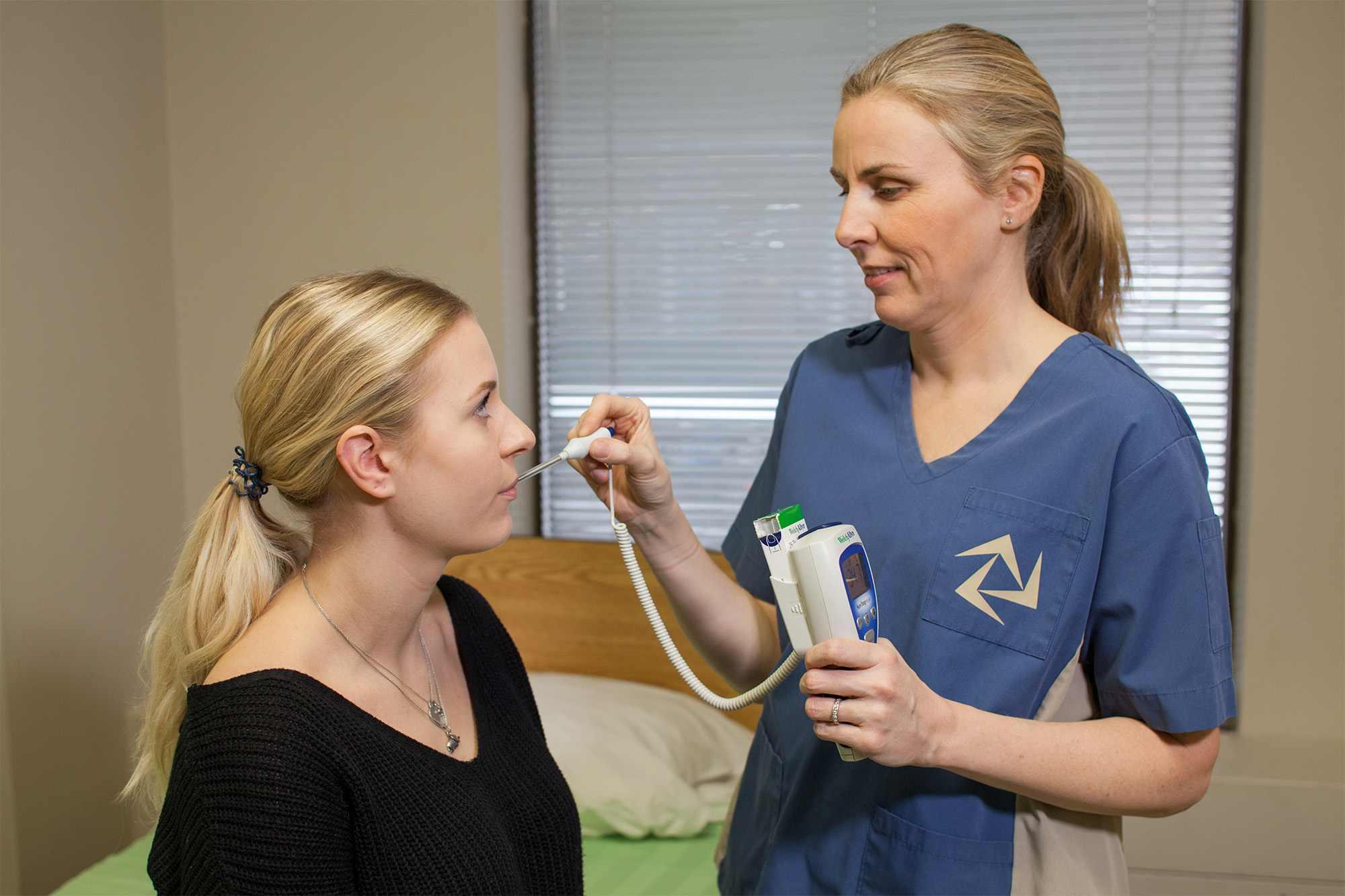
Technique Tips
Putting the probe cover on takes practice. You need to ensure that it snaps onto the probe. Sometimes the device will turn off after you take the probe out of the device if you take too long to put the probe cover on or insert it in the client’s mouth. If so, discard the probe cover and re-insert the probe into the device to reset it. Then try again.
What should the healthcare provider consider?
Healthcare providers often measure the oral temperature, particularly when the client is conscious and can follow directions. Measurement of the oral temperature is not recommended for individuals who are unconscious, unresponsive, confused, have an endotracheal tube secured in the mouth, and cannot follow instructions.
Certain factors render the oral route less accurate with the potential for falsely high or falsely low findings. If the client has recently consumed hot or cold food or beverage, chewing gum, or has smoked prior to measurement, the healthcare provider should use another route such as tympanic or axillary. Selecting an alternate route under the aforementioned circumstances is most conducive to a fast-paced clinical environment and most respectful of the client’s time. If another route is not available, healthcare providers should wait 15 to 25 minutes to take the oral temperature following consumption of a hot or cold beverage/food. The temperature of the beverage/food also factors into the wait period, as extreme heat or cold will require longer wait times for oral temperature assessment. Healthcare providers should wait about 5 minutes if the client is chewing gum or has just smoked since both of these activities can increase temperature.
Test Yourself!
While watching the interactive video on measuring temperature with an oral thermometer, apply your knowledge and critical thinking skills to answer the questions throughout the video. Please note: there is no sound in this video.
Test Your Knowledge
Please answer the three questions in the following question set.
Chapter Attributions
Part of this content was adapted from OER #1 (as noted in brackets above):
- © 2015 British Columbia Institute of Technology (BCIT). Clinical Procedures for Safer Patient Care by Glynda Rees Doyle and Jodie Anita McCutcheon, British Columbia Institute of Technology. Licensed under a Creative Commons Attribution 4.0 International License, except where otherwise noted. Download this book for free at http://open.bccampus.ca

