Interpreting Lab Values
21 Introduction to Interpretation of Lab Values
Lesson
Learning Outcomes
By the end of this chapter, learners will be able to:
- explain types of units used in laboratory testing (Conventional and Standard International Units),
- explain the use of reference ranges and critical values, and
- describe factors which affect the interpretation of numerical lab results.
Units in Laboratory Testing
At times, individuals will have various laboratory (lab) tests taken to aid in monitoring their health. Generally, you will come across lab results measured in Standard International (SI) units. Conventional Units (CU) are used in some settings, particularly in the United States, and so you may come across lab values using conventional units in American learning activities or when reviewing results in a client’s chart if they were transferred from the United States. If you find yourself needing to convert between CU and SI units, there are a variety of conversion charts outlining conversion factors (CF) online. In some lab tests, the type of units used in conventional and SI systems are the same. Included in the table below are examples of differences in types of units used for some common lab tests. Do you recall what the unit abbreviations stand for? Refer back to the conversion table as needed.
| Lab Test | Example for Conventional Units | Example for Standard International Units | Conversion Factor |
|---|---|---|---|
| hemoglobin | 13.4 g/dL | 134 g/L | 10 |
| potassium, serum | 3.9 mEq/L | 3. 9 mmol/L | 1 |
| thyroxine, free | 1.1032 ng/dL | 14.2 pmol/L | 12.871 |
Reference Ranges
When a lab test is measuring an amount of a particular substance in the body, it is typical that normal results will vary slightly between individuals. A reference range shows a spread of possible values you would expect to find for a particular test and is usually reported alongside the results of the lab test.
Serum Potassium Reference Range = 3.5 to 5.0 mmol/L
This means any value below 3.5 is considered low, and any value above 5.0 is considered high.
Therefore, most people have a normal value between 3.5 to 5.0 mmol/L.
These ranges are based on the results of studies which measure the results of a particular lab test in a large number of people. Researchers identify the average result and show the distribution of possible values in a graph. They determine what the standard deviation is for a particular laboratory test and identify values for up to 3 standard deviations away from the average result. Reference ranges usually correlate to the values of 2 standard deviations below and above the average value calculated from the study. This means that some people will have a normal value slightly outside of the reference range.
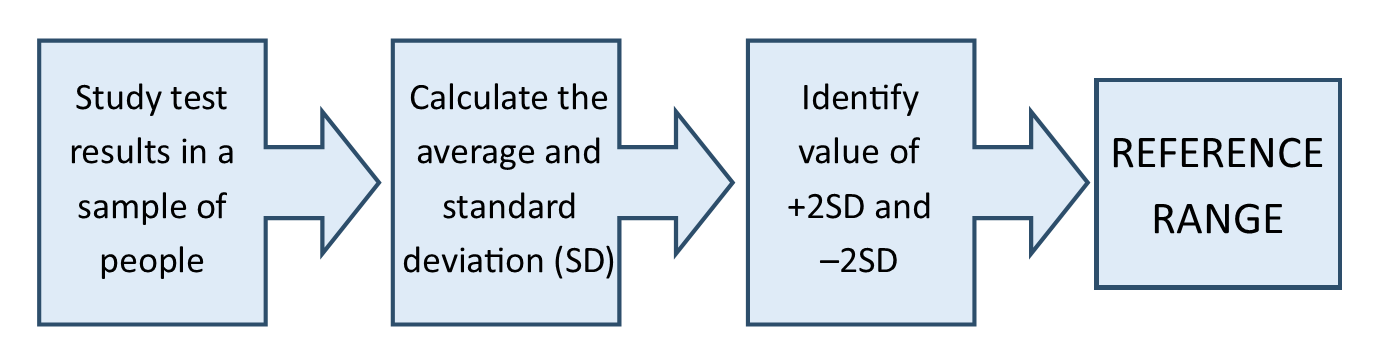
It’s worth noting a study must follow best practice guidelines in order to ensure that the results are valid. For instance, the population sample used in a study should be diverse, so results are not skewed. If a researcher was trying to determine a reference range for hemoglobin and the majority of the study participants had a diagnosis of anemia, the resulting average value of hemoglobin would likely be much lower than if the study participants had a diverse distribution of characteristics which could affect the value being studied. This would not give a good representation of average hemoglobin levels.
Sometimes, there are multiple reference ranges for a particular test because characteristics like age and sex affect the amount of some substances in our bodies. Other factors which can affect laboratory results are time of day or a specific phase of a person’s menstrual cycle. The following tables show some examples where multiple reference ranges are used for a particular test.
| Age | Reference Ranges |
|---|---|
| Newborn | 4.5 to 7.2 mEq/L |
| 2 days to 3 months | 4.0 to 6.2 mEq/L |
| 3 months to 1 year | 3.7 to 5.6 mEq/L |
| 1 year to 16 years | 3.5 to 5.0 mEq/L |
| Adult | 3.5 to 5.0 mEq/L |
| Sex | Reference Ranges |
|---|---|
| Female | ≤ 2.6 nmol/L |
| Male | 6.1 to 27.1 nmol/L |
| Phase | Reference Ranges |
|---|---|
| Midfollicular Phase | 3.9 to 8.8 IU/L |
| Midcycle Peak | 4.5 to 22.5 IU/L |
| Midluteal Phase | 1.8 to 5.1 IU/L |
| Postmenopausal | 16.7 to 113.6 IU/L |
You may notice that reference ranges at particular laboratories may be reported differently from those in a diagnostic manual, as there are some factors which can affect the results of particular tests. For example, arterial blood gas (ABG) results are affected by altitude. Therefore, a laboratory in Banff, Alberta (the city with the highest altitude in Canada) may list their ABG results with a slightly different reference range that Vancouver, British Columbia (at sea level). In other cases, the way that a specific test is processed at an individual laboratory varies, and may result in slightly different test results.
| Source | Adult Female | Adult Male |
|---|---|---|
| Medical Council of Canada | 115 to 155 g/L | 125 to 170 g/L |
| Health Link BC | 120 to 160 g/L | 140 to 174 g/L |
Health Link BC. (2021, December). Complete blood count. https://www.healthlinkbc.ca/tests-treatments-medications/medical-tests/complete-blood-count-cbc
Medical Council of Canada. (2023). Clinical laboratory tests: Adult normal values. https://mcc.ca/objectives/normal-values/
PediaMCU: Cairo University Specialized Pediatric Hospital. (2022). Reference values for children. https://pediamcu.com/172/
Critical Thinking Question
How do you access reference ranges for the clinical practice site you are working in?
Critical Values
In some cases, lab test results may be reported with a warning of a critical value to help alert health care staff of serious results. Critical values always fall outside of the reference range. Results with a critical value may pose an immediate threat to a person’s wellbeing and require urgent intervention to protect health. Depending on the test, there may only be a critical high or a critical low, or a test might have both a critical high and low. It is also possible that a particular test may not have a critical value associated with it, this often happens in cases where results are reported as positive or negative. For instance, a pregnancy test detecting human chorionic gonadotropin (hCG) do not have a critical result. Each health care site and laboratory you work in will have a particular list of critical values they use and a policy and process for responding to critical values.
Serum Potassium Reference Range = 3.3 to 5.0 mmol/L
Critical Low < 3.0 mmol/L
Critical High > 6.1 mmol/L
Critical Values List ARUP Laboratories National Reference Laboratory
Interpreting Lab Values
Reference ranges and critical values are important to understand when interpreting lab results, but they are not the only factors to be considered when determining what the result means for an individual. Interpretation of results often requires knowledge of additional information about the individual’s health history and their care plan. In addition, conversations between members of the interdisciplinary team may be necessary in complex situations. It is also important to be mindful of considering whether or not the test results are accurate. Here are some questions you can ask yourself to guide your critical thinking process when interpreting lab results. Please note that these questions are focused on the interpretation of numerical values of the lab results and do not encompass all of the nursing care and assessments required for patients who have abnormal lab results! Practice exercises in this chapter are focused on individual lab tests, however in actual nursing practice you will often be interpreting results of multiple lab tests in conjunction with each other.
- How does the actual result compare to the result I expected for this person?
- Did I expect the result to be positive or negative, high, low or within the reference range?
- Has the person received a recent intervention which would cause a change in this test result?
- What was the previous result of this test (if it has been done before)?
- What do I know about their current condition and their history that would tell me about why this result was obtained?
- Does this person have a health issue that would impact the result of this test?
- Does the person have assessment findings that correlate with the result of the test?
- How quickly are test results changing?
- How accurate are the test results?
- Was there anything that interfered with any part of the procedure which could impact accuracy?
- Are there any conditions which could cause a false positive or false negative for this person?
- Does this person require follow up care based on the test result?
- What is the person’s goal of care?
- What is the person’s code status?
- Does the person want or need education about the result?
- What kind of monitoring is required?
- What symptoms would I expect to see based on the result of the test?
- Has the person received new orders from the primary care provider?
- What else do I need to know to effectively care for this person?
- Do I need to connect with other members of the interprofessional team?
- What reference materials can I access to increase my understanding related to this topic?
You are caring for a client on the second day after having a total hip arthroplasty. You are following up on the client’s daily hemoglobin test on post op day 2. Here is a sample of how you might use the following prompting questions to interpret the client’s hemoglobin result. We will use the following information to work through this example:
Client MB, male, age 71, full code. No history of bleeding disorders.
Hemoglobin results: Pre op 162 g/L, Post op day 1 125 g/L, Post op day 2 79 g/L, Reference range 125 to 170 g/L.
Pain level 4/10, moderate shadowing to hip dressing. Appears somewhat pale and reports feeling tired today.
- How does the actual result compare to the result I expected for this person?
- Did I expect the result to be positive or negative, high, low or within the reference range? Considering if there was visible bleeding, how saturated the dressing was (the client had moderate shadowing to the dressing) and typical prognosis after a total hip surgery, I expected the client to have a lower value for hemoglobin today. The reference range given by the lab is 125 to 170 g/L. (If you do not see a reference range in a case study question, refer to a diagnostic and lab test manual).
- Has the person received a recent intervention which would cause a change in this test result? I would consider if they had a recent blood transfusion, what typical blood loss is like during a total hip arthroplasty.
- What was the previous result of this test (if it has been done before)? I would refer back to the previous results on the chart-I see the previous results were 162 and then 125.
- What do I know about their current condition and their history that would tell me about why this result was obtained?
- Does this person have a health issue that would impact the result of this test? Yes, they just had a major surgery.
- Does the person have assessment findings that correlate with the result of the test? I would look to see if VS had changed today (particularly drop in blood pressure or increase in heart rate). I’ll observe for skin condition (CWMS) , saturation or shadowing on the dressing and the client’s reported feeling of pain, energy levels and anxiety.
- How quickly are test results changing? Relatively quickly, there was a significant drop both days.
- How accurate are the test results?
- Was there anything that interfered with any part of the procedure which could impact accuracy? no
- Are there any conditions which could cause a false positive or false negative for this person? no
- Does this person require follow up care based on the test result?
- What is the person’s goal of care? To regain mobility post op and be discharged home. I would also need to know if they accept blood products as part of their treatment plan.
- What is the person’s code status? Full code, this indicates I anticipate treatment for low hemoglobin to be given, as warranted by specific test results.
- Does the person want or need education about the result? I would need to ask if the client understood the results given by the primary care provider and/or if they wanted further information.
- What kind of monitoring is required? VS, surgical site and dressing, client’s subjective symptoms, repeat lab work.
- What symptoms would I expect to see based on the result of the test? Potential change in skin colour, becoming paler, fatigue or weakness, possible shortness of breath or other symptoms related to reduced oxygenation to tissues.
- Has the person received new orders from the primary care provider? I would need to check the chart for further orders, anticipating a potential blood transfusion or support with intravenous fluids
- What else do I need to know to effectively care for this person?
- Do I need to connect with others members of the interprofessional team? I need to ensure the primary care physician is aware of the results, I would inform the physio or rehab assistant if they were coming in soon to assist with mobilizing the client.
- What reference materials can I access to increase my understanding related to this topic? Diagnostic test manual, articles related to blood loss and hip arthroplasty.
Sample Exercise 21.1
You are working with a person admitted with dehydration to an acute care medical unit, after experiencing several days of vomiting and diarrhea associated with gastroenteritis. They have a history of chronic renal failure, requiring hemodialysis three times a week on Monday, Wednesday and Saturday. On Friday morning, you receive results from their daily lab work and see their serum potassium result is 5.6 mmol/L. Your nursing instructor asks if you are concerned about this finding. How do you respond? (Use the suggested questions in the section on interpreting lab results to help guide your answer).
For additional information on hyperkalemia refer to the following source: Simon, L. V., Hashmi, M. F., & Farrell, M. W. (2022). Hyperkalemia. In StatPearls. StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK470284/
Answers:
Suggested exemplary response of a senior nursing student, based on the available information (your answer will vary depending on how much you have learned about fluid and electrolyte imbalance, renal failure and dialysis, and the amount of experience you have had in the clinical practice setting):
A serum potassium of 5.6 mmol/L is higher than normal, but I know potassium excretion is impaired in people with chronic renal failure. I also think you can lose potassium when someone has a lot of vomiting and diarrhea with gastroenteritis, so I don’t think the potassium is raised related to their admission diagnosis. I know that dialysis will help to reduce the potassium level, and they are scheduled for dialysis tomorrow. I want to know if this is a typical result for this person because I’m not sure how much their potassium usually increases between dialysis runs. I can check the electronic record to compare to their previous lab results. I wonder if they changed their dialysis treatment on Wednesday because they were worried about them losing too much potassium when they were experiencing a lot of vomiting and diarrhea with their gastroenteritis? I haven’t noticed any symptoms associated with hyperkalemia, but I’ll continue to monitor for muscle pain, weakness or numbness and heart palpitations throughout my shift and report my findings to the primary nurse. Pseudohyperkalemia can occur if the sample wasn’t taken correctly, but if the result is similar to their previous potassium levels on Fridays then I don’t think this is likely (Simon, S. L. et al., 2022). I will see if the physician has seen them this morning yet, and if not discuss the result and treatment plan with them when they arrive. I’m not sure if they would order any medications to reduce the potassium today or check their potassium again before their dialysis run tomorrow. I’m a bit concerned because hyperkalemia can have serious side effects when it starts to get higher, but right now I think I need to check on their previous results to see if this is typical and to see how much it has increased since yesterday. I’m also not sure if the client is on any medications which would increase potassium. Is there anything else I should be considering?
Critical Thinking Questions
- What would you do if a critical result was reported to you while caring for a patient in the hospital?
- Do you think a client with a critical low result will always receive intervention from the healthcare team?
- A male client has a hemoglobin of 124 g/L. How concerned are you? What additional information do you need to consider when interpreting this lab result?
- How do you approach the use of reference ranges for gender diverse clients?
Answers:
- Several things should be considered in related to this question:
- What is your scope, what is your school’s policy, and what is the agency policy?
- Who do you need to communicate this result to and how fast should you be reporting the result? How do you document your communication and actions?
- What should be done in relation the particular result that was critical and the context of the individual?
- Discussion should focus on what is appropriate for the particular individual, and what intervention means.
- Is this the first time the result has been reported, or a repeat result?
- Have interventions been initiated already (prior to the lab test) that we expect will shift the individual’s future results?
- What does intervention look like from various members of the healthcare team? (education, new orders, increased monitoring or assessments, symptom management, etc.)
- What is the goal of care for this person?
- Several factors can influence the significance of this result.
- What is the reference range given by the lab which reported the result?
- What have past hemoglobin levels been for this person?
- What factors do you know of in the person’s history and current condition that might influence the current result?
- Is the person actively bleeding, and if so, by how much?
- At this time, there are no reference ranges specific to diverse gender expressions. As reference ranges are reported as male or female for some tests, a decision must be made to determine if a particular reference range is most appropriate to use for a particular test. The decision might be made by a laboratory staff member, or in partnership with the person’s primary health care provider or specialist, such as an endocrinologist. At other times, the primary care provider might refer to both male and female reference ranges of a particular test. For transgender people, reference ranges will be selected based on the affirmed gender if a person is using gender-affirming hormone therapy (Cheung, 2020). In some cases, gender-affirming hormone therapy will affect the results obtained. For example, erythropoiesis has been found to be affected by treatment with full-dose gender affirming hormone therapy, and tests such as hemoglobin will shift after treatment is started (Cheung, 2020). Tests dependent on organ size may continue to use reference ranges for the person’s assigned sex at birth, such as prostate specific antigen and cardiac troponin (Cheung, 2020). As a student nurse, you should be considerate of the language you are using when providing education and information to people about their lab results to ensure you avoid misgendering people and are sensitive to situations which may be triggering for the person. The article by Irwig (2021) provides an in depth commentary on this topic, and includes ideas for ways to improve health care systems to support better care for transgender and gender diverse patients in relation to effective lab testing.
References:
Cheung, A. S., Lim, H. Y., Cook, T., Zwickl, S., Ginger, A., Chiang, C., & Zajac, J. D. (2020). Approach to interpreting common laboratory pathology tests in transgender individuals. The Journal of Clinical Endocrinology & Metabolism, (106)3, 893-901. https://doi.org/10.1210/clinem/dgaa546
Irwig, S. M. (2021). Which reference range should we use for transgender and gender diverse patients? The Journal of Clinical Endocrinology & Metabolism, 106(3), 1479–1480. https://doi.org/10.1210/clinem/dgaa671
Key Takeaways
- Laboratory results can be reported in Conventional or Standard International Units.
- Conversion factors can be used to convert between the types of units.
- Reference ranges identify the spread of lab values when values fall in a range.
- Reference ranges for a particular test may vary between individual laboratories or for individuals with particular characteristics (eg. age, sex)
- Critical values refer to lab values which fall out of the normal reference range and are considered to be an immediate threat to health.
- Interpreting lab values requires consideration of multiple factors related to the context of the individual.
Practice Set 21.1
Practice Set 21.1: Interpreting blood glucose
You are caring for a client admitted to the acute care medical floor with cellulitis. They have a history of hypertension and type I diabetes.
Admission orders include:
hydrocholothiazide 12.5 mg
insulin aspart SC – see sliding scale QID
glargine 15 units SC OD
ramipril 5mg PO OD
cephalexin 500 mg PO QID
It is the beginning of day shift, 0730, and you have just taken a blood glucose test using the glucometer on the ward to check the client’s blood glucose this morning. The result was 23.2. Use the following suggested questions to discuss the result. Make note of additional information you might need to gather when answering these questions.
- How does the actual result compare to the result I expected for this person?
- Did I expect the result to be positive or negative, high, low or within the reference range?
- Has the person received a recent intervention which would cause a change in this test result?
- What was the previous result of this test (if it has been done before)?
- What do I know about their current condition and their history that would tell me about why this result was obtained?
- Does this person have a health issue that would impact the result of this test?
- Does the person have assessment findings that correlate with the result of the test?
- How quickly are test results changing?
- How accurate are the test results?
- Was there anything that interfered with any part of the procedure which could impact accuracy?
- Are there any conditions which could cause a false positive or false negative for this person?
- Does this person require follow up care based on the test result?
- What is the person’s goal of care?
- What is the person’s code status?
- Does the person want or need education about the result?
- What kind of monitoring is required?
- What symptoms would I expect to see based on the result of the test?
- Has the person received new orders from the primary care provider?
- What else do I need to know to effectively care for this person?
- Do I need to connect with others members of the interprofessional team?
- What reference materials can I access to increase my understanding related to this topic?
Answers:
- You will need to consider if you anticipate the client’s results to be within or outside the reference range. Depending on the client’s use of insulin, food intake, and metabolic needs, you might be able to make a prediction about if there blood sugar should be within, above, or below, the reference range. You should also be comparing the value to the previous blood glucose readings and identify if they have had recent changes in their insulin dose.
- The client has a history of type I diabetes and has a current infection, which can contribute to an increase in blood glucose due to the stress response of the body. You would need to assess for signs and symptoms of high blood glucose to see if the glucose reading correlates to the patient presentation. Has there been a sudden increase in the blood glucose reading? If so, is there anything else you could find from your assessment that would correlate to a sudden increase in blood glucose? For instance, what has your client’s intake been? Did they receive their last dose of insulin?
- Was the test done correctly? Has the blood glucose machine been calibrated? Is the reading at a level that would require a repeat test to confirm accuracy?
- How will the client’s blood glucose be managed? In this case, it needs to be reduced and will require a phone call to the primary care provider to adjust their insulin dose. When will you recheck their blood glucose level? Will you monitor for any additional signs and symptoms? Make sure to check the facility policy on treatment of hyperglycemia. Find out what the client understands about blood glucose during infection. This may be a good opportunity for client teaching.
- In this case, it may not be necessary for intervention from team members other than the primary care provider at this time. You could consider if there is there a need for this client to meet with the diabetic educator, if there is a knowledge deficit requiring further education prior to discharge. Reference materials could include reference to your nursing textbooks, journal articles and hospital policy documents.
Practice Set 21.2
Practice Set 21.2: Interpreting urine drugs of abuse screen
A client is brought to the emergency department with decreased level of consciousness. On arrival the Glasgow coma scale was 12/15. As part of the investigations, a urine for drugs of abuse screen was taken and is positive for opiates. The client’s spouse is adamant the client does not use opiates. No other clear reason for decreased level of consciousness is apparent at this time.
Read the following questions and determine the most important factors to consider for each question.
- How does the actual result compare to the result I expected for this person?
- What do I know about their current condition and their history that would tell me about why this result was obtained?
- How accurate are the test results?
Answers:
- Were there any medications given in the ER which would impact this test result?
- A thorough history, including current prescriptions, must be taken if not already complete. If naloxone was given after the test results were received, did it have any effect on the client’s condition?
- Is it possible to have a false positive for opiates from this test? Yes, there are a variety of over the counter and prescription medications which can cause false positives.
Practice Set 21.3
Practice Set 21.3: Interpreting Arterial Blood Gases
A client is admitted to the hospital with hyperemesis gravidarum during the first trimester of pregnancy. They have vomited multiple times today despite taking antiemetics. Additional symptoms include persistent nausea, fatigue, muscle cramps, and mild disorientation. The client is started on IV fluid to rehydrate and undergoes a variety of diagnostic testing, including examination of arterial blood gases.
pH = 7.46
PaCO2 = 50 mmHg
PaO2 = 97 mmHg
HCO3- = 35 mEq/L
Use the following suggested questions to discuss the result. Make note of additional information you might need to gather when answering these questions.
- Do these results indicate a specific acid-base imbalance?
- How does the actual result compare to the result I expected for this person?
- Did I expect the result to be positive or negative, high, low or within the reference range?
- Has the person received a recent intervention which would cause a change in this test result?
- What was the previous result of this test (if it has been done before)?
- What do I know about their current condition and their history that would tell me about why this result was obtained?
- Does this person have a health issue that would impact the result of this test?
- Does the person have assessment findings that correlate with the result of the test?
- How quickly are test results changing?
- How accurate are the test results?
- Was there anything that interfered with any part of the procedure which could impact accuracy?
- Are there any conditions which could cause a false positive or false negative for this person?
- Does this person require follow up care based on the test result?
- What is the person’s goal of care?
- What is the person’s code status?
- Does the person want or need education about the result?
- What kind of monitoring is required?
- What symptoms would I expect to see based on the result of the test?
- Has the person received new orders from the primary care provider?
- What else do I need to know to effectively care for this person?
- Do I need to connect with others members of the interprofessional team?
- What reference materials can I access to increase my understanding related to this topic?
Answers:
- These results indicate the client is in a state of partially compensated metabolic alkalosis. The pH is high, therefore the client is in a state of alkalosis. Increases in carbon dioxide would shift the pH downwards and increases in bicarbonate would shift the pH upwards. This means the client is in metabolic alkalosis, since the resulting direction of change in pH of an increased bicarbonate level matches the current state of the pH. It is partially compensated as there are changes in carbon dioxide levels without the pH shifting back to a normal level.
- Excessive vomiting can lead to metabolic alkalosis in some severe cases. From the information provided, there are no interventions noted which would cause metabolic alkalosis (eg. excessive gastric suctioning). It is unknown if this patient had previous ABGs taken, and there is no past medical history noted which would affect pH balance.
- The information provided in this case indicates they had persistent, severe vomiting which is a symptom which can lead to alkalosis. Assessment findings which can be associated with metabolic alkalosis include fatigue, muscle cramps and confusion. Therefore, the patient condition correlates with the lab results.
- You may wonder if the sample result is accurate. Results may not be accurate if the test was not collected, stored or handled properly. You might wonder if it was possible that a venous blood sample was taken and not arterial. Aside from double checking with the person who drew the labs and checking to ensure the order was entered correctly you might consider how a venous sample might differ from an arterial sample. Knowing that a venous blood gas would commonly give a lower pH, slightly higher CO2 and bicarb level, it is unlikely to be a venous sample because the pH is higher that normal.
- After reviewing the abnormal ABG results, you should determine how often the client needs reassessment. This can be informed by the frequency of vomiting, the client’s current vitals signs, hospital protocols and types of treatment being provided. At minimum, the client will need to be assessed hourly while receiving intravenous fluid replacement. Check the orders to see if there is a repeat ABG ordered for a particular time or other associated lab test results, such as electrolyte levels. Treatments you should expect are fluid replacement and management of nausea and vomiting. In addition, you could be anticipating what other signs and symptoms and complications you should assess for, such as other electrolyte imbalances or signs of worsening condition, such as further changes in orientation, level of consciousness and signs of seizure activity.
- Review information about collection and interpretation of ABG’s in the hospital lab manual, your nursing textbooks, the hospital library and/or online reference materials.

