Antimicrobials
3.16 Antifungals
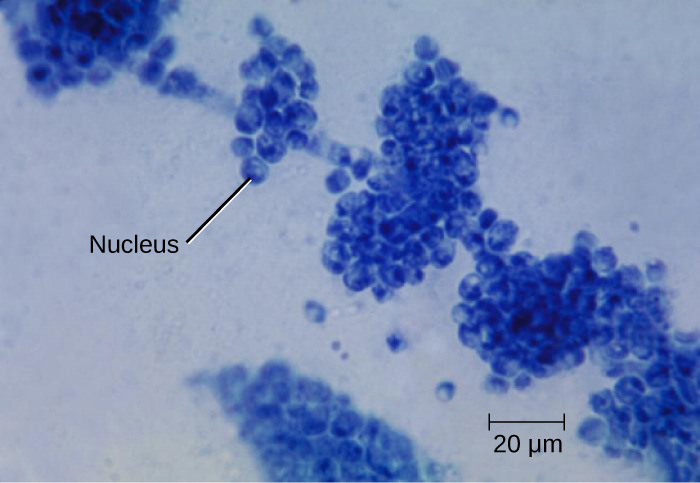
Fungi are important to humans in a variety of ways. Both microscopic and macroscopic fungi have medical relevance, but some pathogenic species that can cause mycoses (illnesses caused by fungi). See Figure 3.13 for a microscopic image of candida albicans that is the causative agent of yeast infections. Some pathogenic fungi are opportunistic, meaning that they mainly cause infections when the host’s immune defenses are compromised and do not normally cause illness in healthy individuals. Fungi are important in other ways. They act as decomposers in the environment, and they are critical for the production of certain foods such as cheeses. Fungi are also major sources of antibiotics, such as penicillin from the fungus Penicillium.[2].
Indications:
Imidazoles are synthetic fungicides commonly used in medical applications and also in agriculture to keep seeds and harvested crops from molding. Examples include miconazole, ketoconazole, and clotrimazole, which are used to treat fungal skin infections such as ringworm, specifically tinea pedis (athlete’s foot), tinea cruris (jock itch), and tinea corporis.
Triazole drugs, including fluconazole, can be administered orally or intravenously for the treatment of several types of systemic yeast infections, including oral thrush and cryptococcal meningitis, both of which are prevalent in clients with AIDS. Triazoles also exhibit more selective toxicity, compared with the imidazoles, and are associated with fewer side effects.[3]
Allylamines, a structurally different class of synthetic antifungal drugs, are most commonly used topically for the treatment of dermatophytic skin infections like athlete’s foot, ringworm, and jock itch. Oral treatment with terbinafine is also used for fingernail and toenail fungus, but it can be associated with the rare side effect of hepatotoxicity.[4]
Polyenes are a class of antifungal agents naturally produced by certain actinomycete soil bacteria and are structurally related to macrolides. Common examples include nystatin and amphotericin B. Nystatin is typically used as a topical treatment for yeast infections of the skin, mouth, and vagina, but may also be used for intestinal fungal infections. The drug amphotericin B is used for systemic fungal infections like aspergillosis, cryptococcal meningitis, histoplasmosis, blastomycosis, and candidiasis. Amphotericin B was the only antifungal drug available for several decades, but its use has associated serious side effects, including nephrotoxicity.[5]
Mechanism of Action: Antifungals disrupt ergosterol biosyntheses of the cell membrane increasing cellular permeability and causing cell death.
Special Administration Considerations: Administration guidelines will vary depending on the type of fungal infection being treated. It is important to monitor response of the affected area and examine class-specific administration considerations to monitor client response.
Client Teaching & Education: The client should be advised to follow dosage instructions carefully and finish the drug completely, even if they feel their symptoms have resolved. The client should report any skin rash, abdominal pain, fever, or diarrhea to the provider. The client should monitor carefully for unexplained bruising or bleeding, which may be a sign of liver dysfunction.[6]
Antifungal Medication Card
Now let’s take a closer look at the medication card for various antifungals in Table 3.15.[7][8][9][10][11][12]
Medication Card 3.16.1: Antifungal
Class: Antifungals
Therapeutic Effects
- Discuss importance of medication compliance
- Monitor response of the affected area
Administration
- Clotrimazole
- Topical cream: apply liberally twice daily to affected area
- Flucanazole
- Route: PO/IV
- Single or multiple doses
- Caution if liver dysfunction
- Terbinafine
- Cream or aerosol
- Wash affected area with soap and water and allow to dry completely before applying
- Nystatin
- PO: If order is “‘swish and swallow,” instruct client to hold medication in mouth for several minutes before swallowing
- Topical cream/powder: apply liberally twice daily
- Amphotericin B
- Route: IV
- Reconstitute and dilute as directed on packaging
- Administer slowly over several hours initially and monitor VS every 30 minutes; may require premedication
- Therapy may take several months
- Alert: Different amphotericin B preparations aren’t interchangeable
- Caution if renal impairment
Indications
- Clotrimazole
- fungal skin infections
- athlete’s foot (tinea pedis)
- jock itch (tinea cruris), or
- Flucanazole
- yeast infections
- Terbinafine
- most commonly used topically for the treatment of dermatophytic skin infections
- Nystatin
- typically used as a topical treatment for yeast infections of the skin, mouth, and vagina, but may also be used for intestinal fungal infections
- Amphotericin B
- for systemic fungal infections like aspergillosis, cryptococcal meningitis, histoplasmosis, blastomycosis, and candidiasis
Side Effects
- Clotrimazole
- topical-skin irritation
- rash
- Flucanazole
- hepatotoxicity
- Terbinafine
- hepatotoxicity
- Amphotericin B
- nephrotoxicity
- hypokalemia
- may be ototoxic.
Therapeutic Effects and Nursing Considerations
- Clotrimazole
- improve symptoms of fungal infection
- Flucanazole
- improve symptoms of yeast infection
- Terbinafine
- Improve symptoms of athlete’s foot (tinea pedis), jock itch (tinea cruris), or ringworm
- Nystatin
- Improve symptoms of yeast infection of skin
- Amphotericin B
- Improvement of systemic fungal infection
- Monitor fluid intake and output; report change in urine appearance or volume
- Monitor BUN and creatinine levels two or three times weekly. Kidney damage may be reversible if drug is stopped at first sign of renal dysfunction
- Hydrate client before infusion to reduce risk of nephrotoxicity
- liver function tests once or twice weekly
- Monitor potassium level closely and report signs of hypokalemia
- Report evidence of hearing loss, tinnitus, vertigo, or unsteady gait
Using the above information, consider the following clinical scenario question:
A client in a skilled nursing facility has been receiving nystatin applied to groin folds twice daily for several weeks, but there is no sign of improvement. What is the nurse’s best response?
Note: Answers to the activities can be found in the “Answer Key” sections at the end of the book.
- This image is a derivative of "Candida albicans" by Dr. Gordon Roberstad, Centers of Disease Control and Prevention. https://cnx.org/contents/y54zcuVm@1/Characteristics-of-Fungi, licensed under CC0 ↵
- This work is a derivative of Microbiology by OpenStax licensed under CC BY 4.0. Access for free at https://openstax.org/books/microbiology/pages/1-introduction ↵
- This work is a derivative of Microbiology by OpenStax licensed under CC BY 4.0. Access for free at https://openstax.org/books/microbiology/pages/1-introduction ↵
- This work is a derivative of Microbiology by OpenStax licensed under CC BY 4.0. Access for free at https://openstax.org/books/microbiology/pages/1-introduction ↵
- This work is a derivative of Microbiology by OpenStax licensed under CC BY 4.0. Access for free at https://openstax.org/books/microbiology/pages/1-introduction ↵
- uCentral from Unbound Medicine. https://www.unboundmedicine.com/ucentral ↵
- Daily Med, https://dailymed.nlm.nih.gov/dailymed/index.cfm, used for hyperlinked medications in this module. Retrieved June 27, 2019 ↵
- UpToDate (2021). Clotrimazole. https://www.uptodate.com/contents/search ↵
- UpToDate (2021). Fluconazole. https://www.uptodate.com/contents/search ↵
- UpToDate (2021). Terbinafine. https://www.uptodate.com/contents/search ↵
- UpToDate (2021). Nystatin. https://www.uptodate.com/contents/search ↵
- UpToDate (2021). Amphotericin B. https://www.uptodate.com/contents/search ↵

